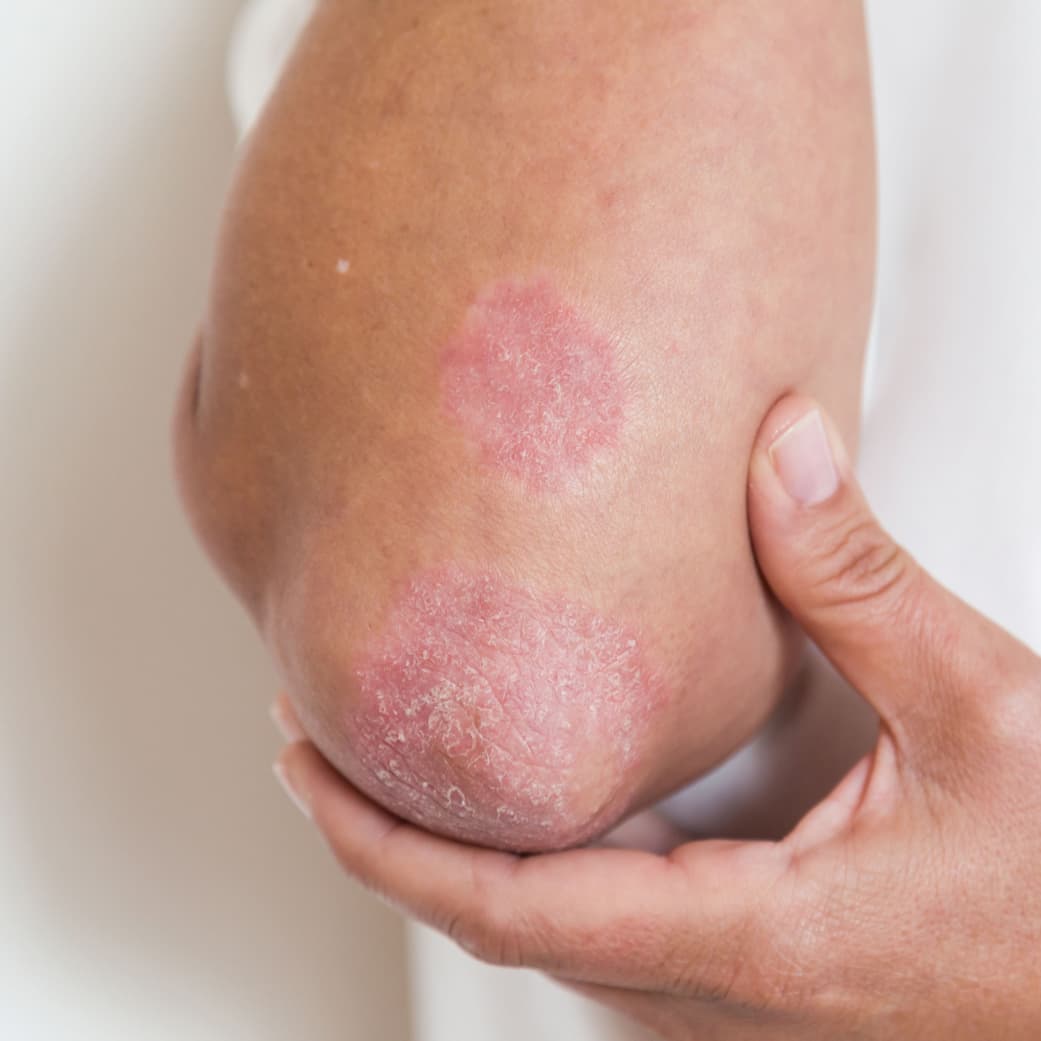
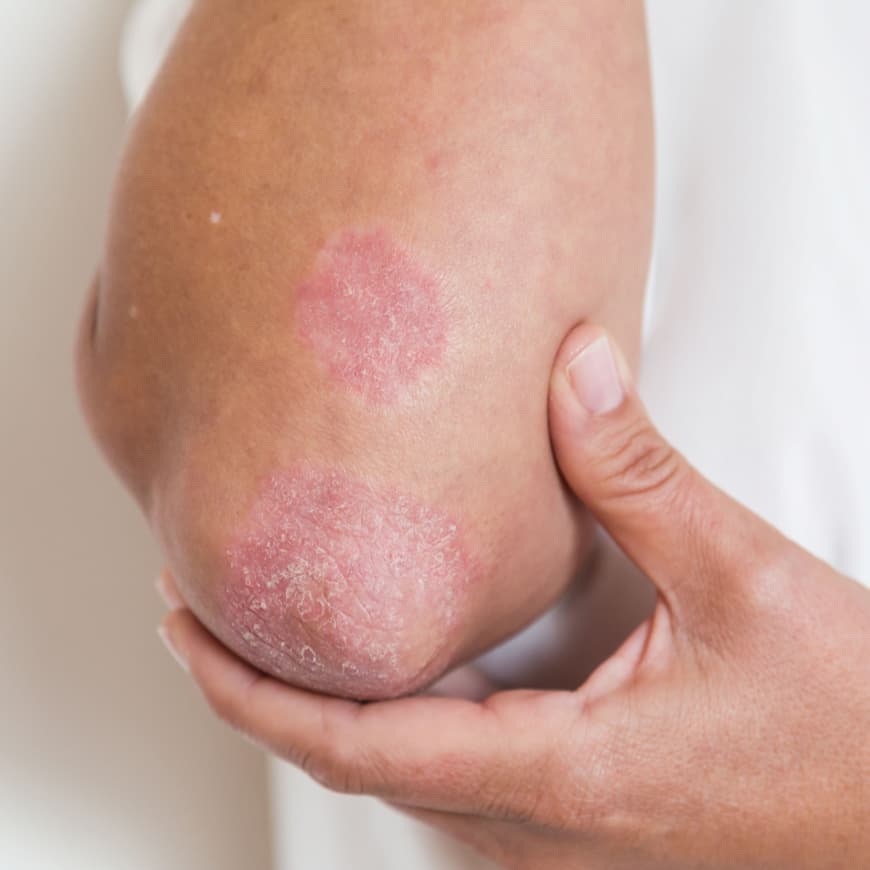
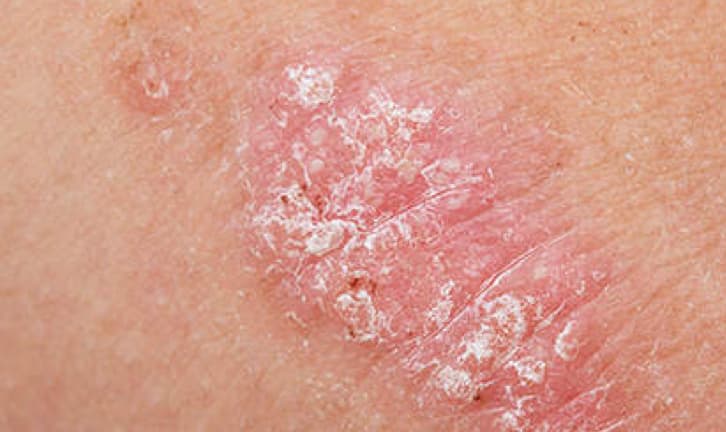
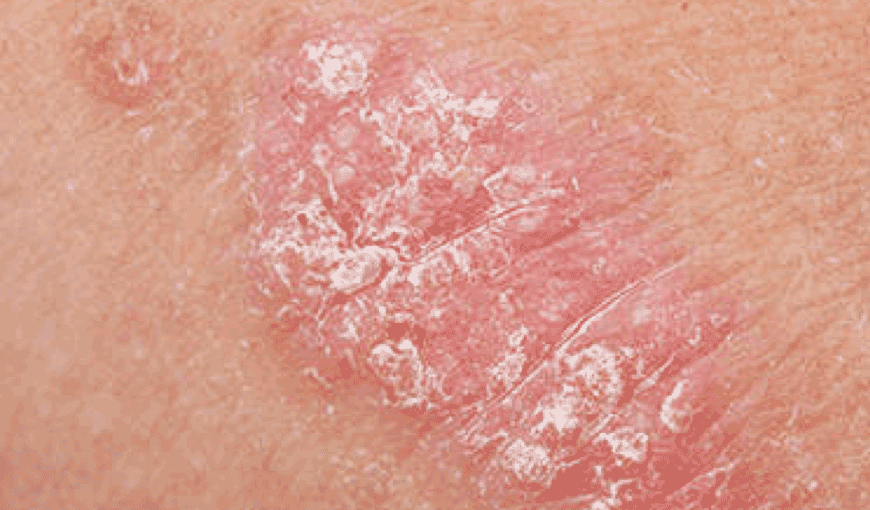
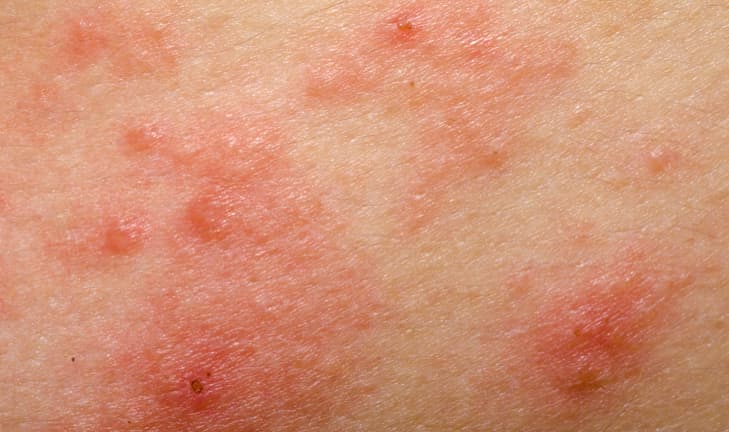
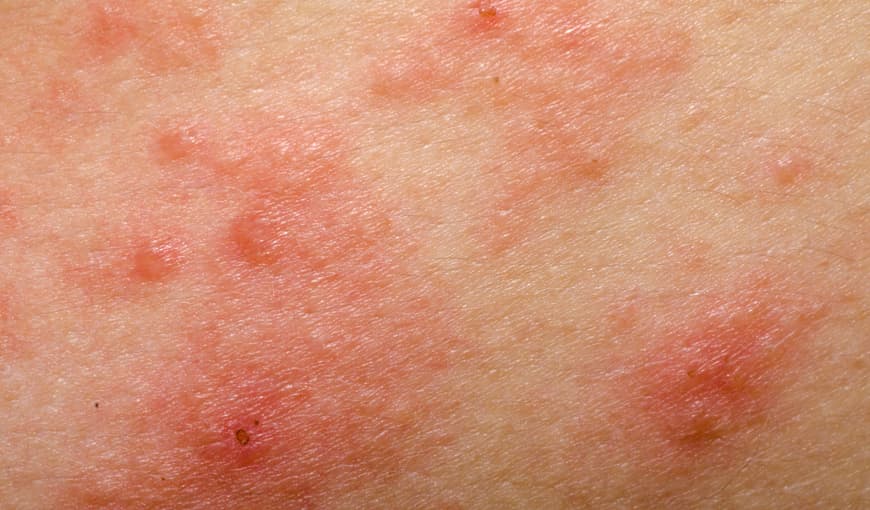
A good place to start learning about psoriasis is beneath the skin’s surface. Many people think of psoriasis as just a skin condition, because that’s where you see and feel the symptoms. Take a closer look, and you’ll see psoriasis is a chronic disease believed to be the result of several factors, including an overactive immune system.
The exact cause of psoriasis is still unknown. However, we do know that inflammation inside the body may cause the symptoms of psoriasis—including the itchy, red plaques you see on the skin.